“The feedback has been heartening. One of the patients said he played this game instead of taking pain medication.”
Dr. Balakrishnan Prabhakaran
Professor of Computer Science
UT Dallas
.…on co-developing the Mr. MAPP VR system for amputees with phantom limb syndrome.
 Dean Peterson, a U.S. Navy veteran who lost his lower left leg 16 years ago after a hunting accident, slept easier for the first time in years when he took part in a recent pilot trial of Mr. MAPP. The “mixed reality” system combines VR and computer vision technologies and was co-developed by Dr. Prabhakaran.
Dean Peterson, a U.S. Navy veteran who lost his lower left leg 16 years ago after a hunting accident, slept easier for the first time in years when he took part in a recent pilot trial of Mr. MAPP. The “mixed reality” system combines VR and computer vision technologies and was co-developed by Dr. Prabhakaran.
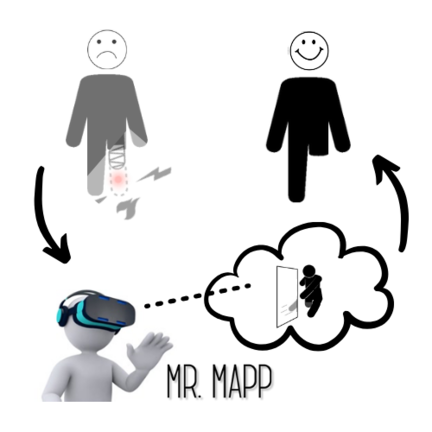
The system uses a laptop, camera, and VR headset to create a virtual 3D model of the user’s missing or paralyzed limb. Wearing the VR headset, Peterson played a series of games where the virtual model of his missing lower leg did things like stomp the floor or burst a bubble.
[Image: VA]
“The whole idea is to fool your brain into actually seeing a leg and foot,” Peterson said in a statement. “By the time I was three weeks into the study, I realized the pain wasn’t bothering me as much at night. It was easier to fall asleep. I was impressed with it.”
Peterson was just one of a dozen veterans who took part in an at-home pilot trial of Mr. MAPP through the Dallas VA Medical Center. Mr. MAPP—short for Mixed reality system for Managing Phantom Pain—was created after years of research led by Dr. Prabhakaran in collaboration with researchers at the Veterans Affairs North Texas Health Care System.
Mr. MAPP uses RGB-D cameras like Microsoft Kinect to turn out a real-time 3D model of the patient. An illusion of their virtual limb is created by mirroring their preserved limb in the captured data, using computer vision and graphics.
Prabhakaran and his fellow researchers see Mr. MAPP as a potential alternative to opioid use—and believe the tech can be used for other conditions that cause pain as well.
A high-tech VR update to a classic therapy

UTD doctoral student Yu Yen Chung with Dr. Prabhakaran [Photo: UTD]
Mixed signals to the brain even many years after an amputation are believed to be the cause of phantom limb pain. The Mr. MAPP system is designed to help the brain resolve the signals. It’s an update to the classic “mirror box therapy” treatment, which uses a box and a mirror to give the patient the illusion of their missing limb. But the box and mirror therapy isn’t ideal, Prabhakaran says, and is usually only offered in health care settings.
Using VR and augmented-reality technology—which overlays real-world objects into virtual settings—Mr. MAPP improves on the treatment, while letting patients use Mr. MAPP themselves right in their own homes.
Peterson had tried mirror box therapy unsuccessfully in the past, which is why he’s excited by Mr. MAPP’s potential.
“It was a pretty cool feeling. It felt like I had two feet, and that was cool enough that I wanted to stick with it,” Peterson said.
Senior author Prabhakaran and the study’s co-authors described Mr. MAPP in an article published online October 22 in Pilot and Feasibility Studies.
UT Dallas co-authors of the study include Kanchan Bahirat, Ph.D., who worked on the project as a doctoral student and now works at Simbe Robotics, and Yu Yen Chung, a computer science doctoral student. Other contributors include corresponding author Dr. Thiru Annaswamy, formerly with UT Southwestern Medical Center and the Dallas VA and recently named chair of physical medicine and rehabilitation at Penn State Health Milton S. Hershey Medical Center; Dr. Gargi Raval, assistant professor of physical medicine and rehabilitation at UT Southwestern; and Tri Pham, a UT Southwestern medical student.
For more of who said what about all things North Texas, check out Every Last Word.
![]()
Get on the list.
Dallas Innovates, every day.
Sign up to keep your eye on what’s new and next in Dallas-Fort Worth, every day.
























